Breast Lift
What is the goal of a breast lift?
A breast lift, or mastopexy, can raise sagging breasts, elevate drooping nipples, and make large areolas smaller. Mastopexy is a trade-off of improved shape for permanent scars. There is no change in the appearance of the breasts when clothed and supported by a bra. Mastopexy procedures can also enlarge the breasts if implants are added at the same time.
How much lift can I expect from a mastopexy?
The short answer is not as much as most would like. It is not possible to raise the breasts enough to completely eliminate all overhang. Mastopexy is accomplished by pushing the breasts up from below in order to restrict scars to the lower half of the breasts. This is an inherently less powerful approach than what most women demonstrate by pulling their breasts up from above while raising their arms to simulate what they expect from the procedure. However, in appropriate candidates mastopexy can raise the breasts significantly while improving skin tone, breast shape, and areolar aesthetics.
There is another thing that mastopexy cannot do. It will not help women with long torsos and breasts that are naturally positioned low but otherwise exhibit good shape and minimal sag. The breasts cannot be moved to a higher position on the chest by any type of surgery.
Who is a candidate for mastopexy?
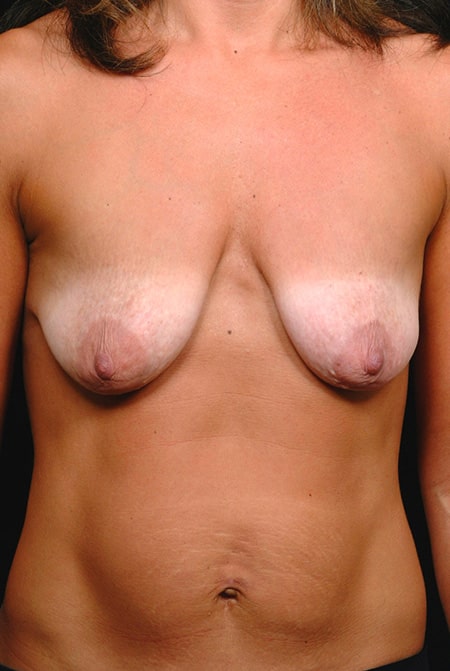
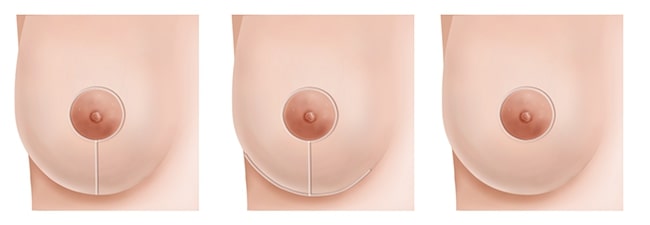
Mastopexy is most commonly performed in postpartum patients with breasts that have sagged from multiple pregnancies and breast feeding. A deflated look is typical, with stretch marks, downward pointing nipples, and enlargement of the areolas (Figure 1).
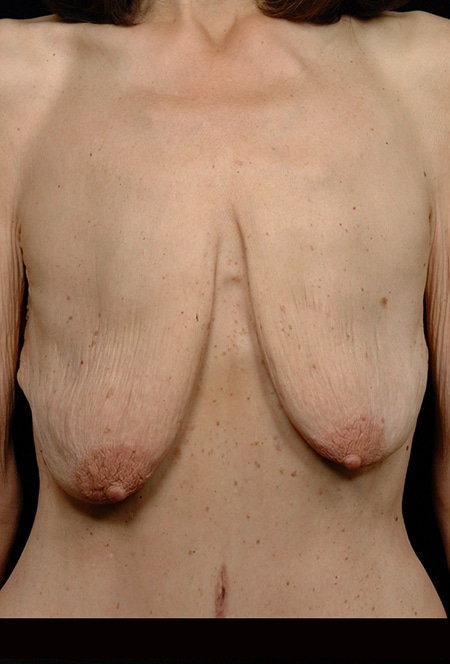
Those experiencing massive weight loss following gastric bypass and other forms of bariatric (weight loss) surgery are also excellent candidates for mastopexy. These individuals usually exhibit the most severe conditions (Figure 2).
Women in their twenties who have not been pregnant and are interested in a breast lift are usually not good candidates for surgery. Their conditions are usually mild and do not justify creating the scars necessary.
When should mastopexy be performed?
A mastopexy should be considered only when there is no longer the prospect of additional pregnancies. Individuals who have experienced massive weight loss should be at a stable weight for at least six months prior to seeking surgery.
How is a mastopexy done?
In a standard mastopexy skin is removed from the lower part of the breast in order to conceal the scars as much as possible. It is not surgically possible to lift the breasts from above without creating profound and objectionable scars. In addition to removing excess skin the nipple position is raised during mastopexy. Contrary to a common misconception the nipple and areola are not disconnected from the breast at any time during surgery. Instead, the skin is rearranged around them in such a way that they are pushed upward once all of the incisions are closed.
The visible portion of the final scar pattern in mastopexy encircles the areola and courses downward from the bottom of the areola to the crease under the breast (Figure 3). The most traditional type of mastopexy also includes a long scar in the crease under the breast.
The breast tissue deep to the skin can be rearranged during mastopexy in order to shift more of it into the upper, empty part of the breast. This offers the prospect of a fuller upper breast contour. However, this option is much more invasive and the recovery not as simple as with procedures that only involve skin tightening. Furthermore, these more invasive procedures have never really been proven to be more effective than skin tightening alone.
An alternative method of increasing upper breast fullness at the time of mastopexy is to add implants at the same time. Combining mastopexy with breast augmentation is more complex: it takes longer to do, has more of a recovery, costs more, and is subject to the all of the potential problems associated with implants.
What are the different options available?
The most common type of breast lift used today is called a vertical mastopexy. It has a “lollipop” scar pattern that courses around the areola and then vertically down to the bottom of the breast (Figure 4, left). This method can be used for most patients. The more traditional breast lift option is called an inverted-T mastopexy and has an “anchor” scar pattern. This procedure creates a long scar in the crease under the breast in addition to the lollipop pattern (Figure 4, center). This method is reserved today for those with more extreme amounts of excess breast skin, such as seen following massive weight loss.
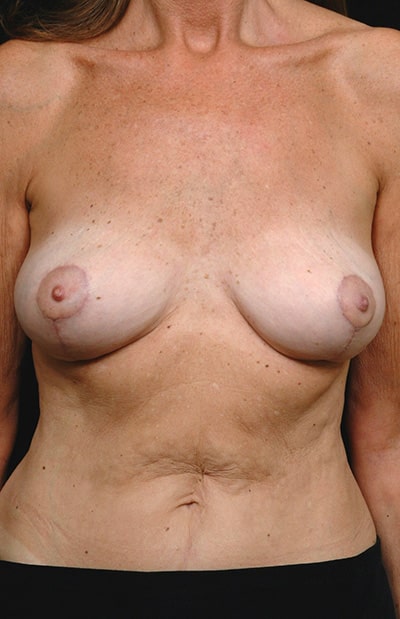
Internal lifting of the breast tissue can be done in many different ways. All include dividing the glandular tissue into portions and then rearranging it to push the breast mass upward. There is no consensus in the field as to which method is best. All make breast lifts more complex and substantially lengthen surgery time. Furthermore, as already stated, there are no scientific studies to prove that any of these internal lifting methods add long term benefit beyond what skin tightening alone can accomplish.
A breast lift can be limited to a scar just around the areola (Figure 4, right). However, this method is not very powerful. Moreover, the scar around the areola often becomes thick and wide due to high skin tension around the areola inherent with this technique. This approach can be useful as an adjunct to breast augmentation where it can make a large areola smaller or raise nipple position slightly.
What size will my breasts be after mastopexy?
Breast size will be exactly the same as before unless implants are added.
When are implants used with breast lifts?
Small breast implants can be used to fill in a hollow upper breast that would otherwise remain following mastopexy alone. Breast size does not increase significantly in this instance but the previously empty part of the bra is filled out. It is also possible to substantially increase breast size with implants during mastopexy, typically going up by at least one cup size.
What do the scars look like?
The vertical scar is usually the most noticeable because it is not hidden in a crease or disguised by the areola. Scars may spread in response to skin tension no matter how meticulously the incisions are closed. This is particularly true for scars around the areola when they are the only scars present.
All scars are permanent but they usually fade considerably by one year. Their final width, texture, and color commonly vary from person to person.
Will I still need to wear a bra after surgery?
It will remain necessary to wear a bra after a breast lift. Surgically lifted breasts are not immune to the chronic effects of gravity, the downward forces associated with impact exercise, and activities such as horseback riding. However, bras are more comfortable to wear after surgery because they are no longer required to lift the breasts but rather just hold them in place.
What about nipple sensation and the ability to breast feed?
A breast lift consisting only of skin removal is extremely unlikely to diminish nipple sensation. More invasive procedures that internally lift the breast or combine augmentation with mastopexy have a greater chance of adversely affecting nipple sensation. Sometimes nipples become unpleasantly hypersensitive after surgery. This particular condition is a benign process that eventually resolves.
The ability to breast-feed normally after a breast lift is similar to the sensation issue: more invasive procedures that involve dividing the breast tissue are more likely to impair function. This particular issue is not a common concern because most women do not seek a breast lift until after their last pregnancy.
How long do the benefits of surgery last?
Poor skin elasticity, large breast size, future pregnancies, and weight gain can cause the breasts to slowly sag again. If this should occur the skin can be retightened with a second procedure that is smaller in scope than the original and does not create new scars. However, most women have a long-lasting improvement after a breast lift and do not require repeat surgery.
Where is the surgery performed and how long does it take?
Breast lifts are performed in the office as an outpatient procedure. The procedure takes about two and a half hours. Including implants adds at least another hour. All surgery is performed entirely by Dr. Hidalgo.
Can other procedures be done at the same time?
A breast lift without augmentation can be combined with other aesthetic procedures such as eyelid surgery, rhinoplasty, liposuction, or a facelift, for example. The determining factor for combining a breast lift with other procedures is the total operating time entailed. Up to six hours is a reasonable limit. Since a breast lift with augmentation takes substantially longer than a breast lift alone, there are greater limits on adding other procedures at the same time.
What type of anesthesia is used?
General anesthesia is required. A board certified anesthesiologist is present for the entire procedure and uses state-of-the-art monitoring equipment.
What are the risks associated with a breast lift?
Bleeding, infection, loss of nipple or skin tissue, decreased nipple sensation, delayed healing and excessive scarring can occur following a breast lift, but all are quite rare. Combining implants with a breast lift adds the risks associated with implants. Among the more significant ones are capsular contracture (implant hardening) and uneven positioning of the implants. Both can require corrective surgery. In addition, implants require periodic replacement throughout life.
Why is smoking so harmful for surgery?
Smoking severely reduces blood supply to the breast tissue and skin. It delays healing and can be responsible for skin or nipple loss, wound infection, bad scars, and other complications that may require corrective surgery. It is therefore essential to stop smoking completely for at least three weeks before surgery and six weeks after. Simply cutting back is not enough. Nicotine containing patches and gum are equally harmful.
What is the recovery like?
The pain associated with a breast lift tends to be mild. Most women report discomfort along the incision lines that is well controlled by oral medication. Breast lifts combined with implants have more discomfort for the first forty-eight hours due to implant placement under the pectoral muscle.
A simple surgical bra that opens in the front is worn for one week. Regular bras with wires can be worn after that. There are no drains to remove. Skin stitches dissolve and do not require removal.
Most activities that do not involve lifting and carrying heavy items can be resumed after one week, including return to work. Flying and driving are not recommended for two weeks. Mild cardiovascular exercise without impact such as a stationary bike can begin gradually at two weeks. More intense exercise can resume at six weeks but activities such as jogging, weightlifting, ball sports, yoga, pilates, skiing, and horseback riding should be delayed for two months.
What are the costs involved in having surgery?
There are separate fees for surgery, anesthesia, operating room use, and for breast implants, if applicable. Costs also include preoperative lab tests and medical grade photographs.
What are the steps involved in proceeding with surgery?
At the initial consultation your breast anatomy will be evaluated and a specific surgical plan proposed, provided that you are a good candidate for one of the available options. Once the plan is agreed upon a surgical date can be scheduled. Photographs and preoperative laboratory studies follow. Women over forty, or those over thirty-five with a family history of breast cancer, should have a mammogram prior to surgery if it has been over a year from the previous study.